


The US Healthcare Industry is a costly market due to high physician, hospital stay, labs and procedure charges along with insurance premiums.
Members enrolled in an insurance program often do not take steps to maintain their health conditions. This leads to an increased number of hospital admissions and higher expenses for the payers.
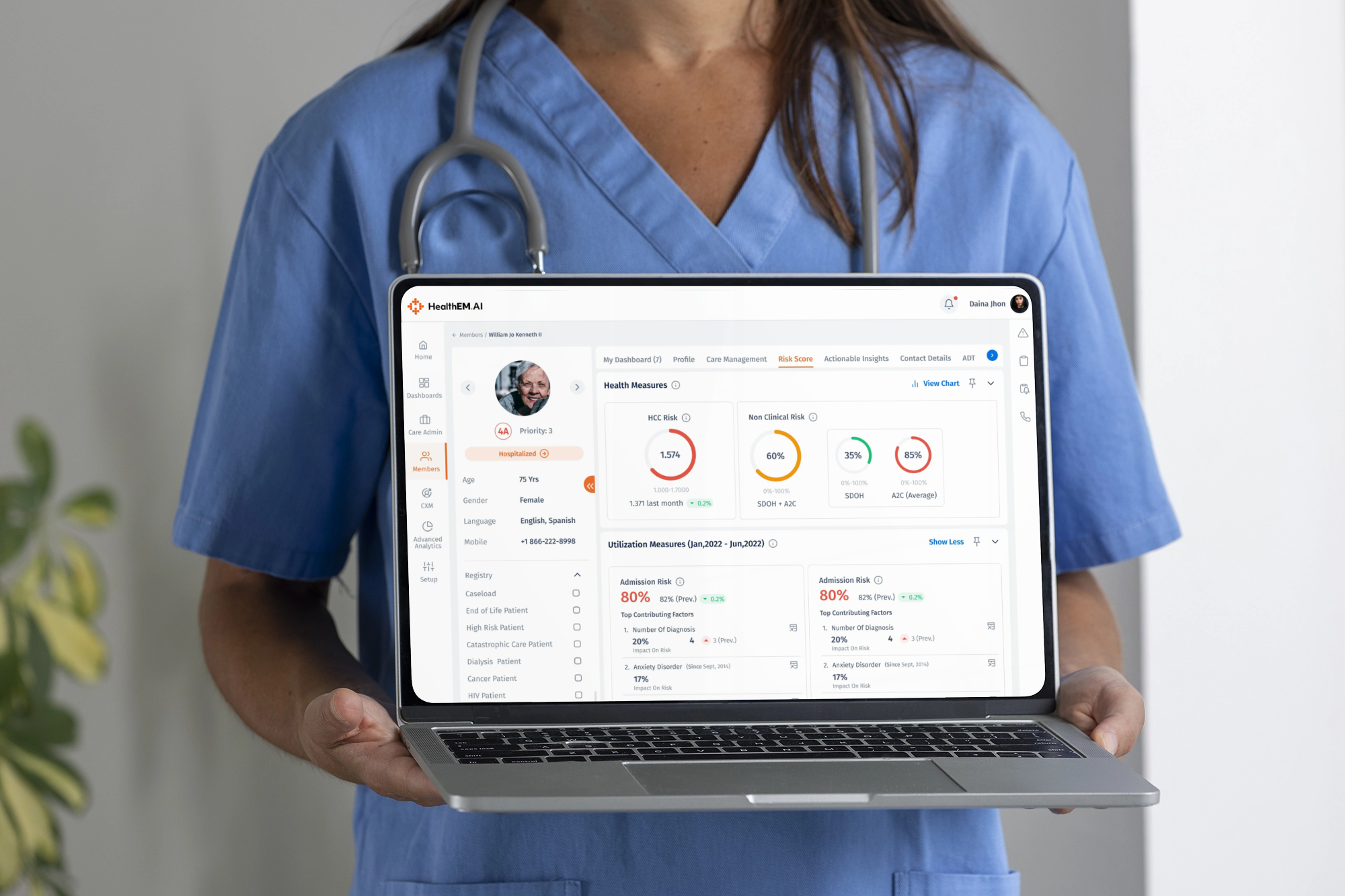
HealthEM.AI was designed to bridge this gap — a platform that helps care managers proactively track, engage, and improve member health outcomes.
Members enrolled in an insurance program often do not take steps to maintain their health conditions — leading to increased hospital admissions and higher expenses.
Despite gathering vast amounts of data, care managers struggle to utilize it effectively due to disconnected systems, leading to inefficiencies and reduced quality of care.
Care managers handle hundreds of patients. Lack of proper prioritization makes it difficult to focus on high-risk individuals first.
Information is scattered across different tabs and systems, requiring excessive clicking to get a full picture of a patient's health.
Logging calls, assessments, and follow-ups takes too much time away from actual patient interaction.
Administrators struggle to track team performance and reallocate caseloads without tedious manual reviews.
The healthcare industry has three key stakeholders whose objectives often conflict.
Health plan providers, Medicare, and Medicaid — that set service rates, collect premiums, and reimburse medical claims.
Members enrolled in insurance plans and patients admitted to hospitals whose treatments payers are covering.
Doctors, Nurses, Clinics, Labs, Hospitals, and Old age homes that provide care to patients.
A structured approach from research to final delivery.
Stakeholder interviews, contextual inquiry, user segmentation, and competitor analysis to understand the landscape.
Persona creation, journey mapping, information architecture, and identifying design directions based on research insights.
Wireframing, UI style guide, visual design, prototyping, and usability testing with real users.
Design system documentation, developer handoff, and iterative improvements based on user feedback.
Five distinct user roles were identified through stakeholder interviews and contextual inquiry sessions.
Nurses onboarded for tracking and health management of members
Head of Care Managers responsible for staff management and team goals
Medical professionals acting as the first point of consultation for patients
Healthcare administrators overseeing effective management of the system
Responsible for company turnover through strategic reports and decisions
Deep-dive into our primary users to understand their goals, frustrations, and daily workflows regarding care management.





"Maintaining accurate documentation of all calls while building trust is overwhelming without clear performance metrics."
"Reviewing team performance across programs and assigning individual patients to CMs is highly tedious."
"Multiple CMs taking up the same patient reduces our overall efficiency and causes confusion."
"I want to help the elderly take care of themselves so nobody feels alone during a time of need."
Derived from client workshops, competitor analysis, and persona research.
Integrate all data and functionalities into one holistic platform ecosystem, reducing workflow friction.
Automated intelligence logic to assist care managers in day-to-day tasks.
Suggestive advanced search.
Contextual guides aligned to data.
Member details logically grouped to decrease system-level cognitive load and improve navigation speeds.
Data structures supported with automated graphs and visual status coding.
Dynamic hover features drop the massive cognitive load.
Beautiful tracking of white space and absolute minimal design elements to ensure natively crisp information mapping.
Restructuring the navigation and module hierarchy to ensure that care managers can find patient data with minimal clicks.
Forgot password, Help, Password expired, Lockouts
Primary navigation hierarchy
Building a trustworthy experience through consistent typography and thoughtful colors.
Polished, production-ready interfaces built with real data, semantic colors, and intuitive information hierarchy.
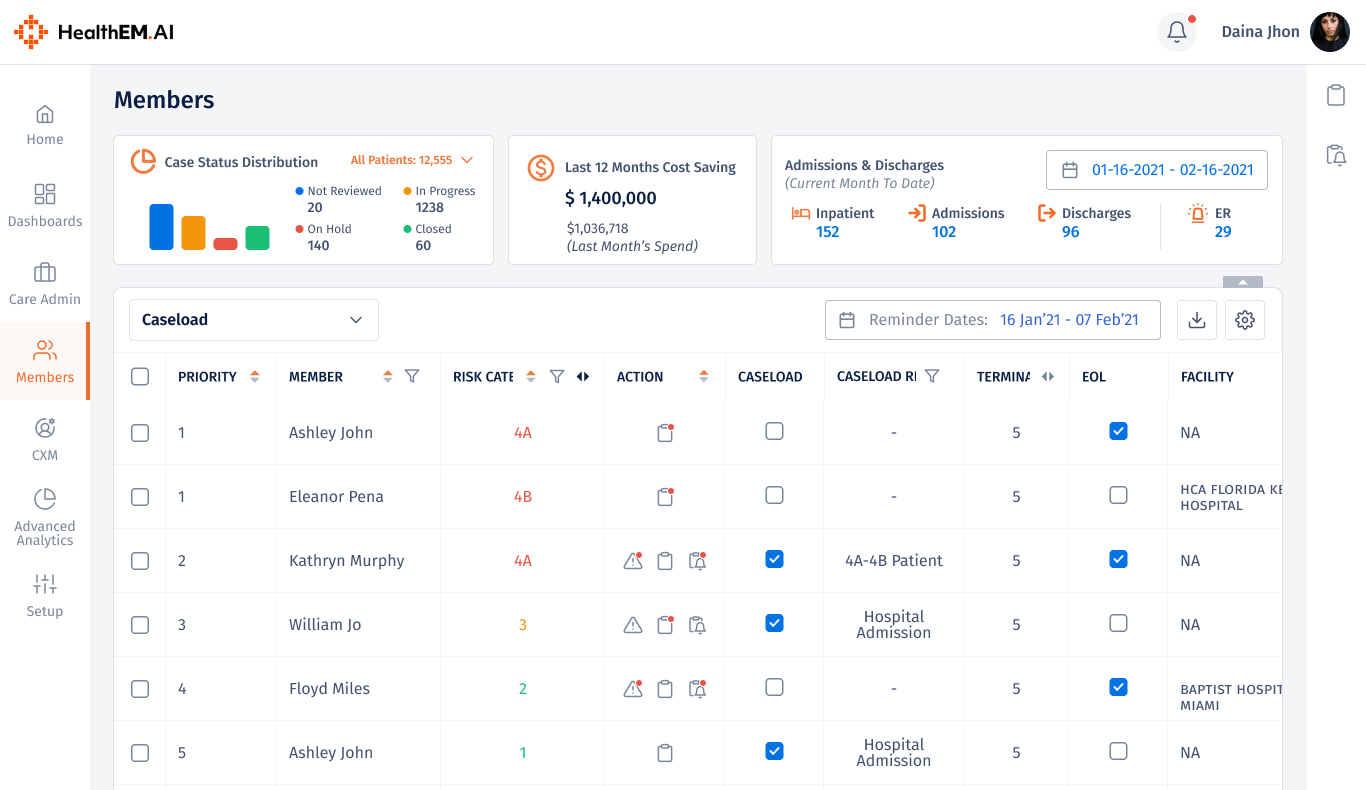
A centralised view of all members across the care network. Care managers can filter by case status, risk level, and assigned physician — reducing time spent hunting for the right patient.
An in-depth profile combining medical history, care tasks, upcoming appointments, and real-time cost data. Designed to give care managers everything they need in a single, structured view.
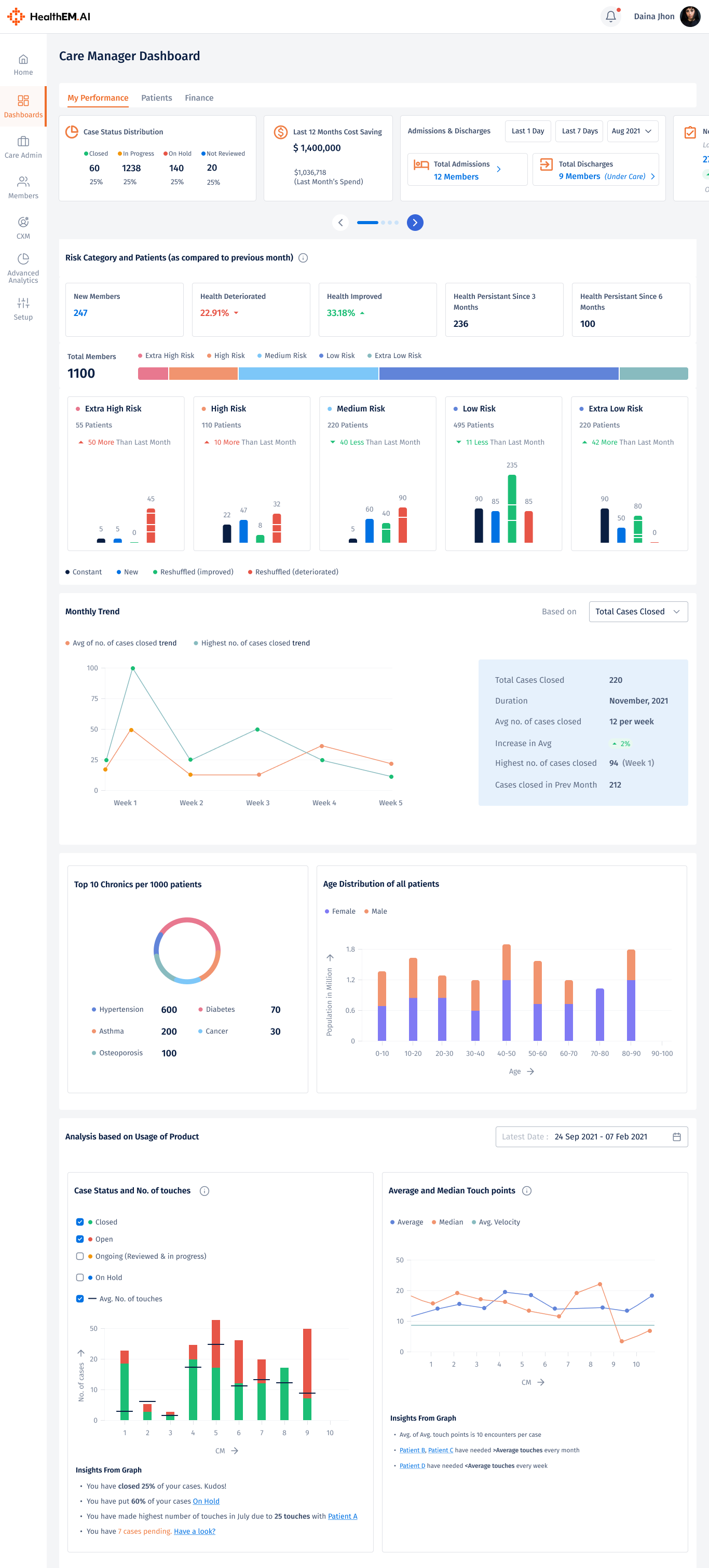
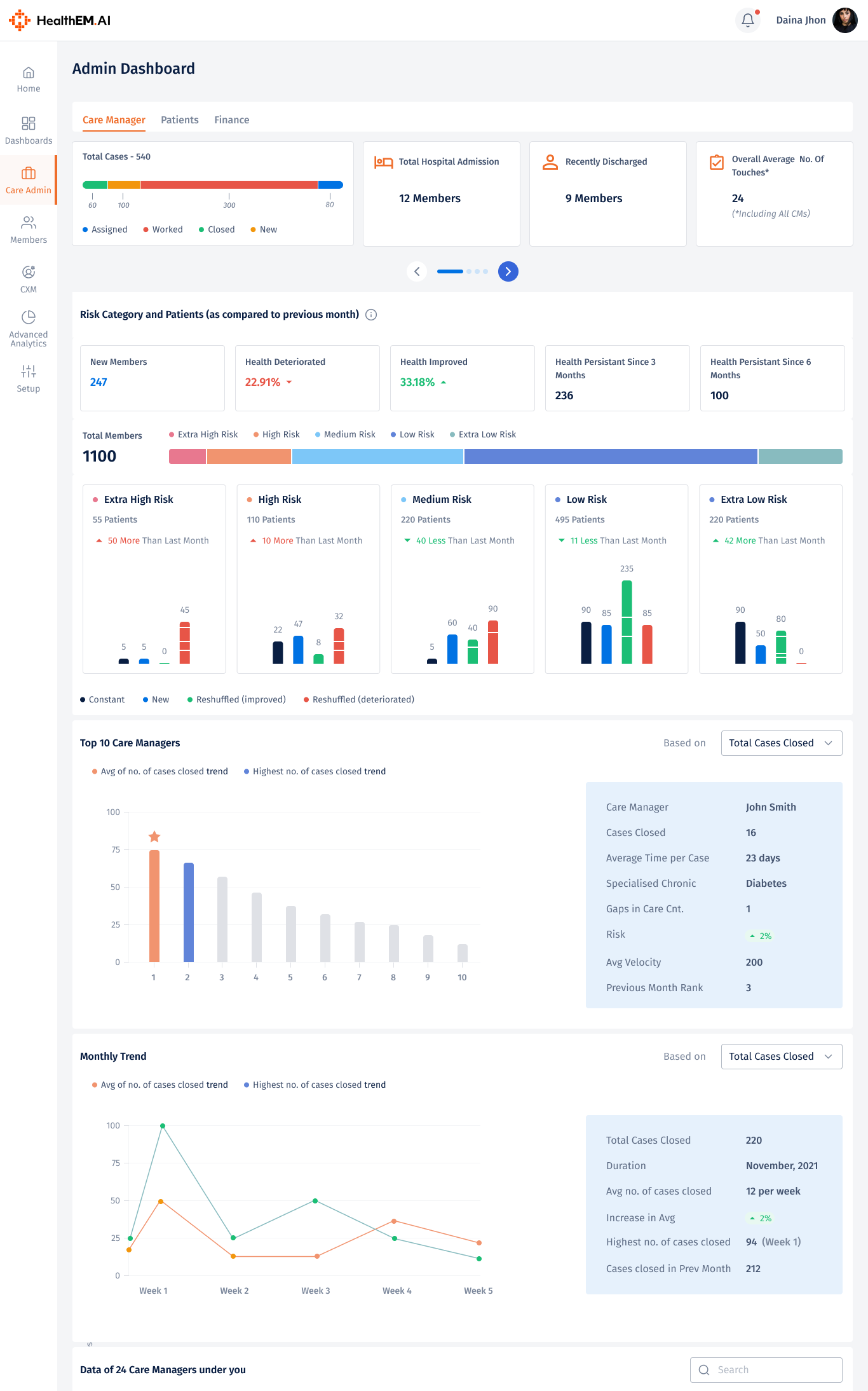
Executive-level visibility into team performance, case throughput, and cost savings. Built for CMOs and CXOs to track KPIs and make informed strategic decisions without leaving the platform.
A personalised workspace showing each care manager's active caseload, task completions, and upcoming follow-ups. Prioritises urgent actions so nothing critical slips through the cracks.